FYP Weekly Report:
Week 2/13 – 25/8/2017
Student: Douglas Lim Jun Siang
Supervisor: Peer M Sathiskh
What have I done?
- Working on the Feedbacks.
The following are the set of questions and comments given by the PD professors and schoolmates:
Target Group Suggestion:
- Be specific on your target group.
- Different types of illness, different types of effects and different types of needs.
- There are different stages of immobility so which level are you looking at? Why?
My research objective is to identify my target group for this project and understand their many needs.
The definition of an elderly:
Under Singapore statistics, people at the age of 65 and above is classified as an elderly.
The cause of elderly immobility:
The following is the list of common disease and illness:
Physical
Musculoskeletal disorders
Arthritis
Osteoporosis
Fractures (especially hip and femur)
Podiatric problems
Neurological disorders
Stroke ( Top 4 killer in Singapore)
Parkinson’s disease ( Increasing patients in recent years)
Other (cerebellar dysfunction, neuropathies)
Cardiovascular disease
Congestive heart failure (severe)
Coronary artery disease (frequent angina)
Peripheral vascular disease (frequent claudication)
Pulmonary disease
Chronic obstructive lung disease (severe)
My project will be focusing on elderly at the aged of 65 and above. The types of illness that I am working on is Osteoarthritis.
Mobility is a key aspect to achieve an active aging. The effect immobility can lead to
Aging, is not the only factor that cause immobility.
Degeneration of the body cells and organs leads to poor immune system. Therefore, leading other common illnesses and diseases to be developed and contributes to immobility.
I want to create a device that helps these patients because they need more attention. This is the first step of toward building a mobility device that replace wheelchair. Fight the pain by giving the elderly the confidence that they can do it.
What is Osteoarthritis?



Osteoarthritis or degenerative joint disease is the most common form of arthritis. Initially it affects the joint cartilage, causing pain in the joints. The pain and stiffness in the joint can ultimately restrict movement. The pain tends to get worse towards the end of the day and with activity.
The primary cause of osteoarthritis is increased age and “wear and tear” of the joints. However, there is increasing research evidence that osteoarthritis may be more than just “wear and tear”.
Osteoarthritis can also arise as a side effect of other problems that put abnormal stress on the joints, such as obesity (from the joints having to carry that extra weight), abnormally shaped hips and knees (added stress is placed on these joints when a person moves), a previous fracture or injury involving the joint, or in the case of some sportsmen, repeated stress to the joint.
Who gets affected?
Osteoarthritis affects both men and women with women having a higher rate of osteoarthritis. Osteoarthritis rates increase sharply after the age of 50.
What are the risk factors for Osteoarthritis?
Osteoarthritis is linked to age, obesity, sports injuries, hereditary (especially osteoarthritis of the hands) and may be associated with other forms of arthritis like rheumatoid arthritis and gout.
Can Osteoarthritis develop in all joints?
Almost any joint can be affected. However, Osteoarthritis commonly develops in the knees, hips, spine, and hands.
What are the symptoms of Osteoarthritis?
The first symptom of Osteoarthritis is a recurring pain in the affected joint(s) or muscles around the joint after a period of prolonged or strenuous use, such as after a long walk or exercise. The pain increases with continued use of the joint, but usually subsides after sufficient rest.
Mild stiffness usually sets in when the joints have been rested (“gelling”). Therefore, if you’ve been sitting still for some time, your hips and knees may feel stiff upon standing again.
In advanced Osteoarthritis where much of the cartilage or “protective lining” around the joints has disintegrated, it may cause an increased secretion of joint fluid, which tends to accumulate around the joint area leading to mild swelling of the joint.
What happens to the joints in Osteoarthritis?
Our joints are normally covered with cartilage so that they can glide over each other smoothly. In Osteoarthritis, the joint cartilage steadily softens and disintegrates over time.
With the loss of this protective material, the exposed bones of the joint begin to grind against each other more easily and wear each other out, creating a painful sensation when weight is put on them, such as during walking or standing up.
As the condition progresses, cysts, bony lumps and excess fluid may develop in the affected joint, giving rise to a swollen joint.
How is Osteoarthritis diagnosed?
If a patient exhibits the symptoms of Osteoarthritis, the doctor can confirm the diagnosis by doing a physical examination and X-rays. The degenerative effects of Osteoarthritis on the bones of the joint will show up clearly on the X-ray.
Sometimes, additional tests and procedures may be needed:
- Magnetic resonance imaging (MRI)
– may be used to get a better picture of the condition of the joint.
- Joint aspiration
– may be carried out to obtain a sample of the fluid in the joint.
- Arthroscopy
– a procedure in which the interior of the joint is visualised by using a special instrument.
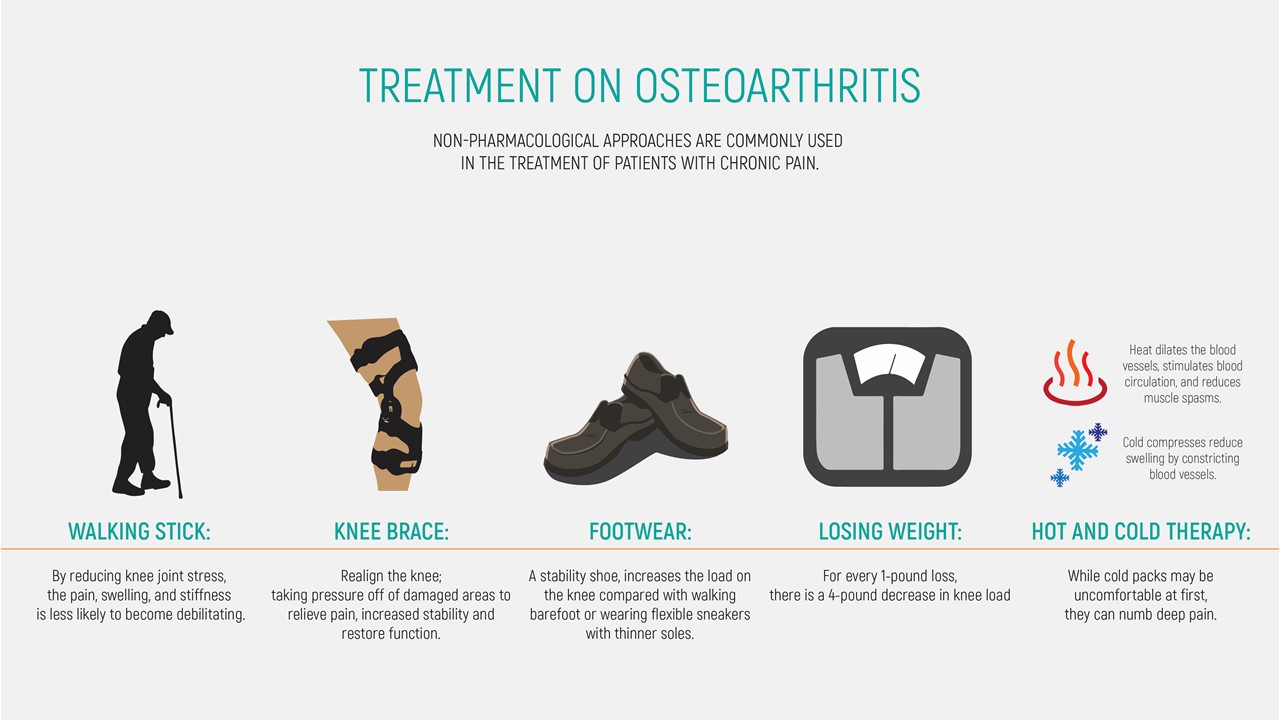
What is the treatment for Osteoarthritis?
There is currently no cure for osteoarthritis. However, there is evidence that OA is not just due to ‘wear and tear’. Hence, sustained and increasing research is necessary. Treatment of osteoarthritis centers on alleviating its symptoms, regaining lost muscle strength and surgery.
- Medication
Most medications treat only the symptoms of Osteoarthritis. Paracetamol (Panadol) can be prescribed for low-level pain, while stronger drugs like non-steroidal anti-Inflammatory drugs (NSAID) and COX-2 inhibitors may be necessary for more severe pain. The effect of glucosamine and chondroitin is variable. Speak to your doctor first before you try these supplements.
If movement becomes significantly affected, steroids or hyaluronic acid preparation may be injected directly into the joint. The effect is usually temporary and cannot be used in the long term as they can cause adverse side effects.
- Physiotherapy
Physiotherapy is needed to build up the strength in the surrounding muscles so that they can hold up the joint better, lessening the stress and strain that is exerted on the joint.
Exercises such as walking (with an aid, if necessary), swimming or cycling are recommended for most forms of arthritis.
- Surgery
In advanced cases, surgery may be required to remove bone fragments, realign the joints, or even replace the joint with an artificial part.
Are Osteoarthritis and Rheumatoid Arthritis similar?
Both are arthritic conditions, but the causes are different. Rheumatoid Arthritis arises out of the body’s immune system attacking its own tissues, while primary Osteoarthritis is caused by wear and tear of the joints.
What are the complications of Osteoarthritis?
The condition can be debilitating and sufferers may be at some risk of depression. Severe Osteoarthritis can result in joint deformity.
Can Osteoarthritis be prevented?
One cannot prevent ageing. One can however reduce the risk of developing Osteoarthritis by maintaining a healthy weight, engaging in moderate exercise and eating a healthy and nutritious diet. Early diagnosis and treatment can prevent further joint damage and deformity.
After researching on the types of illness and disease, physical mobility is essential to strengthen and boost the quality of active aging.
Why Osteoarthritis instead of other illness?
Of all the diseases and illness, Osteoarthritis will be commonly faced by Singaporean in future.
Here the top three reasons why?
1. Young and Active People are getting Osteoarthritis
- Poor lifestyle
- Osteoarthritis cannot be prevented.
Possible Design Direction:
Prevention Measures:
- Maybe it can be an education system to prevent mobility issues.
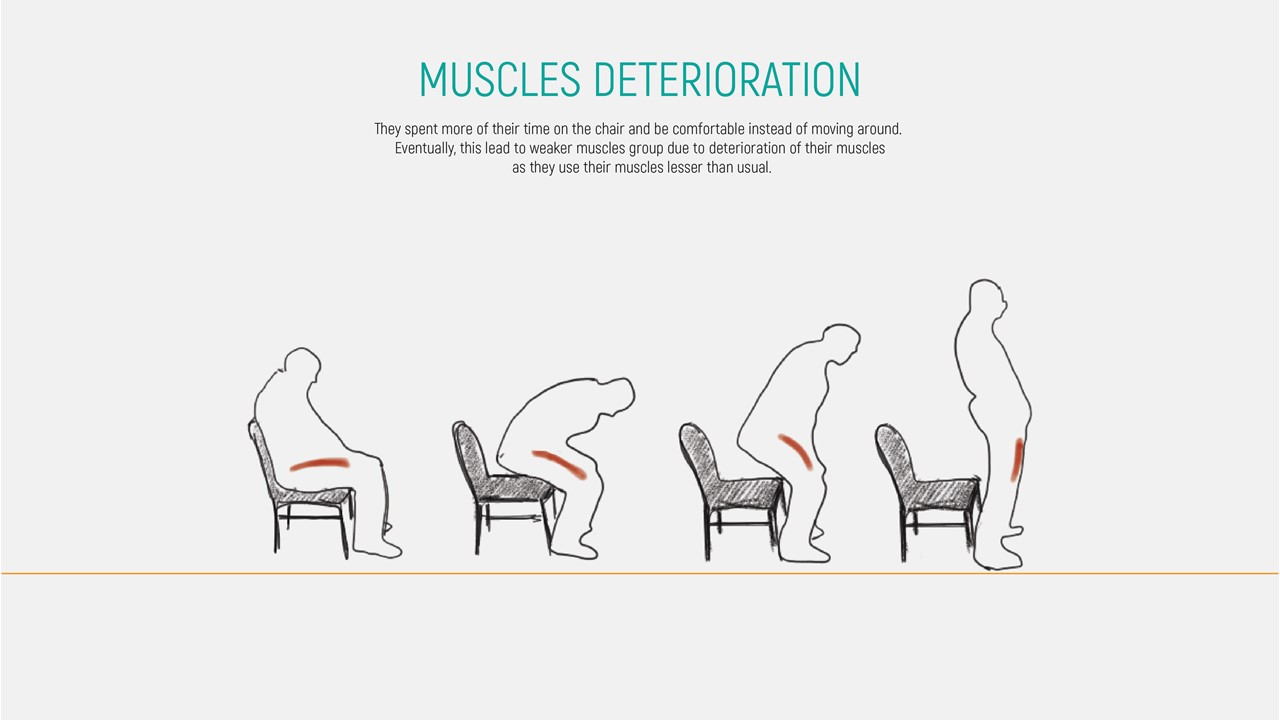
- Create a chair that people will want to reject being on it.
Responsive Measures:
- As for People who already have this mobility issue I want to give them another alternative. If they choose to be wheel chair bound, so be it. For those who yearns to achieve more things, my design can help. It’s a matter of choice.
Product Function:
- Able to enhance their physical ability
- Able to take more steps
- Able to walk longer distance
- Able to overcome the traffic light before it goes red.
Other comments:
- Aging is part of life
- What you reap, what you sow.
- Elderly wants to do things by themselves.
- Actions Taken:
Following actions made:
- Emailed to the respective centres to be a volunteer.
- Talk to people
Interact with the following personnel
- Doctors
Two training doctors gave two different opinions in terms of mobility issues.
These are their inputs.
The problems that I would like to work on is …
It is a degenerative disease on the joint
- Elderly
Interview with Mr Gong
Mr Gong Profile:
Point A to Point B

Activity chart: Sitting, standing, walking.
i. Where does the weight land on?
ii. What kind of the impact are we looking at?
iii.When is the painful part?
Key takeaways:
- Infographics:
- After having all the information required, I created the following infographics to make the information easier to understand and less dense.
- Pain :
- As we are unable to experience the pain from the elderly, it generates other different effects that worse the experience.
- Different Expectation:
- The elderly I spoke to have a certain expectation on how they lived their life. They already knew what is ahead for them and there is nothing for them to expect. Except for more disease to strike and take them away.
Bibliography
After hip fracture, exercise at home boosts day-to-day function. (14 March , 2014). Retrieved from Harvard Health Publications Harvard Medical school : https://www.health.harvard.edu/blog/after-hip-fracture-exercise-at-home-boosts-day-to-day-function-201402197041
Hennie CJP Janssen, M. M. (25 August, 2017). The American Journal of Clinical Nutrition. Retrieved from Vitamin D deficiency, muscle function, and falls in elderly people1,2: http://ajcn.nutrition.org/content/75/4/611.full
National Library Education & Outreach. (03 September , 2017). Retrieved from Singapore Aging population: http://www.nlb.gov.sg/sure/ageing-population/
Schwab, K. (31 8, 2017). Why You Should Be Designing For Your 73-Year-Old Self. Retrieved from Co.Design: https://www.fastcodesign.com/3067220/why-you-should-be-designing-for-your-73-year-old-self







































 Sources: Pinterest ( Mobility, Robotic, Art Concepts)
Sources: Pinterest ( Mobility, Robotic, Art Concepts)




















